Abstract
Background
Sepsis is the leading cause of morbidity and mortality in newborns. CD64 combined
with c-reactive protein (CRP) could improve the sensitivity and specificity of neonatal
sepsis diagnosis, but the results were still controversial. Therefore, this meta-analysis
was conducted to clarify the importance of CD64 combined with CRP in the diagnosis
of neonatal sepsis.
Methods
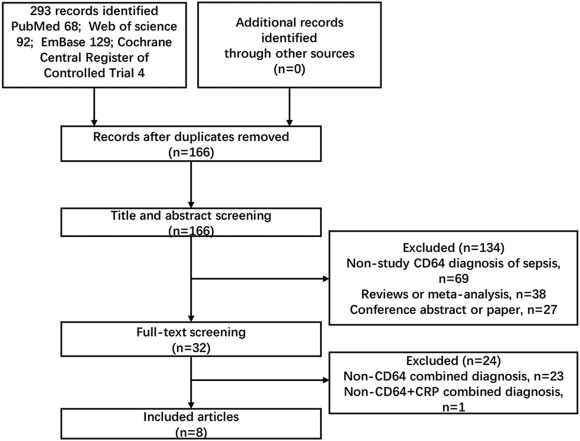
The researches published as of December 24, 2018 were comprehensively searched in
PubMed, Embase (included Embase and Medline), the Cochrane Library and Web of Science.
Totally, 8 articles were included, involving 1114 objects. Statistical calculations
were performed using Stata14.0 and Review Manager 5.3.
Results
The diagnostic accuracy of all included studies was pooled as follows: sensitivity,
0.95 (95% CI: 0.86–0.98); specificity, 0.86 (95% CI: 0.74–0.93); positive likelihood
ratio (PLR), 6.8 (95% CI: 3.50–13.20); negative likelihood ratio (NLR), 0.06 (95%
CI: 0.02–0.18); diagnostic odds ratio (DOR), 118.0 (95% CI: 25.00–549.00), and the
area under the curve (AUC) was 0.96 (95% CI: 0.94–0.97). It was found that heterogeneity
was not caused by threshold effect (P = 0.16), but the results of sensitivity (I2 = 87.57%) and specificity (I2 = 89.07%) analyses indicated significant heterogeneity between studies.
Conclusions
The combined application of CD64 and CRP improved the accuracy of neonatal sepsis
diagnosis.
Keywords
To read this article in full you will need to make a payment
One-time access price info
- For academic or personal research use, select 'Academic and Personal'
- For corporate R&D; use, select 'Corporate R&D; Professionals'
Subscribe:
Subscribe to The American Journal of Emergency MedicineAlready a print subscriber? Claim online access
Already an online subscriber? Sign in
Register: Create an account
Institutional Access: Sign in to ScienceDirect
References
- Global, regional, and national causes of child mortality in 2000-13, with projections to inform post-2015 priorities: an updated systematic analysis.Lancet. 2015; 385: 430-440
- Strengthening the Reporting of Observational Studies in Epidemiology for Newborn Infection (STROBE-NI): an extension of the STROBE statement for neonatal infection research.Lancet Infect Dis. 2016; 16: e202-e213
- Diagnosis of neonatal sepsis: a clinical and laboratory challenge.Clin Chem. 2004; 50: 279-287
- Neurodevelopmental and growth impairment among extremely low-birth-weight infants with neonatal infection.Jama. 2004; 292: 2357-2365
- Usefulness of a semi-quantitative procalcitonin test kit for early diagnosis of neonatal sepsis.Singapore Med J. 2008; 49: 204-208
- Procalcitonin used as a marker of infection in the intensive care unit.Crit Care Med. 1999; 27: 498-504
- Neutrophil CD64 as a diagnostic marker of sepsis: impact on neonatal care.Am J Perinatol. 2015; 32: 331-336
- Neutrophil CD64 as a sepsis biomarker.Biochem Med (Zagreb). 2011; 21: 282-290
- Role of neutrophil CD64 index as a screening marker for late-onset sepsis in very low birth weight infants.PLoS One. 2015; 10e0124634
- Translational research and biomarkers in neonatal sepsis.Clin Chim Acta. 2015; 451: 46-64
- Effective biomarkers for diagnosis of neonatal Sepsis.J Pediatric Infect Dis Soc. 2014; 3: 234-245
- Early-onset neonatal sepsis.Clin Microbiol Rev. 2014; 27: 21-47
- Neutrophil CD64 expression as a longitudinal biomarker for severe disease and acute infection in critically ill patients.Int J Lab Hematol. 2016; 38: 576-584
- Ratio of neutrophilic CD64 and monocytic HLA-DR: a novel parameter in diagnosis and prognostication of neonatal sepsis.Cytometry B Clin Cytom. 2016; 90: 295-302
- Neutrophil CD64 as a diagnostic marker for neonatal sepsis: meta-analysis.Adv Clin Exp Med. 2017; 26: 327-332
- Meta-analysis of diagnostic accuracy of neutrophil CD64 for neonatal sepsis.Ital J Pediatr. 2016; 42: 57
- Expression of miR-18a and miR-210 in normal breast tissue as candidate biomarkers of breast cancer risk.Cancer Prev Res (Phila). 2017; 10: 89-97
- Bivariate analysis of sensitivity and specificity produces informative summary measures in diagnostic reviews.J Clin Epidemiol. 2005; 58: 982-990
- Quantifying heterogeneity in a meta-analysis.Stat Med. 2002; 21: 1539-1558
- Measuring inconsistency in meta-analyses.Bmj. 2003; 327: 557-560
- The performance of tests of publication bias and other sample size effects in systematic reviews of diagnostic test accuracy was assessed.J Clin Epidemiol. 2005; 58: 882-893
- Value of combined determination of neutrophil CD64 and procalcitonin in early diagnosis of neonatal bacterial infection.Chinese Journal of Contemporary Pediatrics. 2017; 19: 872-876
- Significance of neutrophilic CD64 as an early marker for detection of neonatal sepsis and prediction of disease outcome.Journal of Maternal-Fetal and Neonatal Medicine. 2017; 30: 1709-1714
- Neutrophil CD64 combined with PCT, CRP and WBC improves the sensitivity for the early diagnosis of neonatal sepsis.Clin Chem Lab Med. 2016; 54: 345-351
- Diagnostic utility of neutrophil CD64 as a marker for early-onset sepsis in preterm neonates.PLoS ONE. 2014; 9
- Evaluation of adhesion molecules CD64, CD11b and CD62L in neutrophils and monocytes of peripheral blood for early diagnosis of neonatal infection.World J Pediatr. 2012; 8: 72-75
- Predictive values of neutrophil CD64 expression compared with interleukin-6 and C-reactive protein in early diagnosis of neonatal sepsis.J Clin Lab Anal. 2010; 24: 363-370
- Neutrophil CD64 is a sensitive diagnostic marker for early-onset neonatal infection.Pediatr Res. 2004; 56: 796-803
- Neutrophil CD64 expression: a sensitive diagnostic marker for late-onset nosocomial infection in very low birthweight infants.Pediatr Res. 2002; 51: 296-303
- Diagnosis and management of bacterial infections in the neonate.Pediatr Clin North Am. 2004; 51 ([viii-ix]): 939-959
- Diagnostic tests in neonatal sepsis.Curr Opin Infect Dis. 2008; 21: 223-227
- Umbilical blood biomarkers for predicting early-onset neonatal sepsis.World J Pediatr. 2012; 8: 101-108
- Interleukin-6 for early diagnosis of neonatal sepsis with premature rupture of the membranes: a meta-analysis.Medicine (Baltimore). 2018; 97e13146
- The accuracy of the procalcitonin test for the diagnosis of neonatal sepsis: a meta-analysis.Scand J Infect Dis. 2010; 42: 723-733
- Inflammatory markers in cord blood or maternal serum for early detection of neonatal sepsis-a systemic review and meta-analysis.J Perinatol. 2014; 34: 268-274
- The combination of procalcitonin and C-reactive protein or presepsin alone improves the accuracy of diagnosis of neonatal sepsis: a meta-analysis and systematic review.Crit Care. 2018; 22: 316
Article Info
Publication History
Published online: May 03, 2019
Accepted:
May 2,
2019
Received in revised form:
April 2,
2019
Received:
January 31,
2019
Identification
Copyright
© 2019 Published by Elsevier Inc.